18 Apr Removal of Essure Contraceptive Device
An increasing number of women with the Essure contraceptive device are requesting its removal. In this blog, we will cover what the Essure device is, why women are seeking its removal, and how we can remove it safely. Dr Kent Kuswanto is a specialist gynaecologist in Melbourne helping women everyday with gynaecology related issues.
What is the Essure contraceptive device?
Essure is a permanent birth control device that is implanted in the Fallopian tubes. It was used in thousands of women from 1999 up until its withdrawal from the market in 2017.
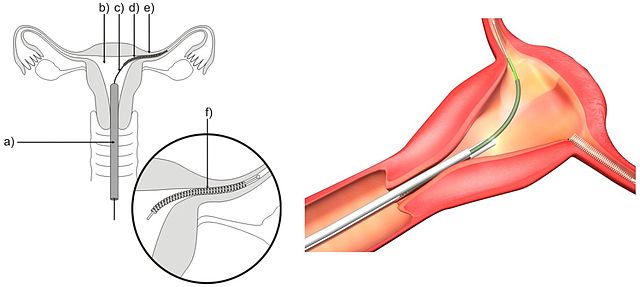
Essure contraceptive device was marketed as a non-surgical non-hormonal minimally invasive contraceptive alternative to tubal ligation or salpingectomy (surgical cutting, clipping, blocking or removal of Fallopian tubes). A gynaecologist usually performed this procedure in either a clinic under local anaesthetic or in a hospital under general anaesthetic. The gynaecologic surgeon did not need to make any incision in the abdomen. He or she would insert a hysteroscope – a thin telescope attached to a video camera and light source – through the cervix and into the uterus. The Essure device is then introduced into each of the Fallopian tubes from the uterine cavity.
The device is a soft flexible metal coil that is made of materials that include polyester PET fibres, nickel, titanium, platinum, silver-tin and stainless steel. Over the next few months, scar tissue forms around the coil, which in turn blocks the Fallopian tube and creates a barrier that prevents sperms from reaching the egg. This results in permanent contraception.
Why are women seeking removal of Essure?
Following reports of side effects and complications in some women with Essure devices in Australia and worldwide, the Therapeutic Goods Administration in August 2017 advised Australian hospitals and doctors to stop using the Essure device. Essure is no longer being sold or inserted in Australia.
The majority of women who have Essure inserted for permanent contraception do not have any issues with the device. However, some women with the Essure device have reported persistent long term side effects from it. Some of these symptoms may be local within the uterus and pelvis, other symptoms may be systemic and varied in nature.
Local symptoms may include:
- Abdominal or pelvic pain
- Abnormal periods
- Severe bloating
- Cramping in the implant location
- Pain during sex
Women have also reported these systematic symptoms:
- Brain fog, dizziness and fainting
- Fatigue
- Allergic symptoms such as itching, swelling, rash or hives.
- Migraines
- Weight gain
- Changed toilet habits
- Joint aches
- Depression
- Autoimmune disease
- Hair loss
While these symptoms may not be easily and readily linked to having an Essure device, there are now many advocacy groups raising awareness of the potential risks and side effects in women with Essure. With this raised awareness, many women are now seeking removal of Essure in order to avoid further complications and improve their overall health and quality of life.
How is the Essure device removed safely?
Most women with an Essure device have no reportable symptoms related to it. It works well in preventing unplanned pregnancy in women who have completed their family and as such, removal of the device is not required. In women with symptoms that may be related to Essure, however, surgery is required to remove the device.
Essure was not designed to be removed. As a permanent irreversible birth control device, it works by causing scar tissue to form around its coil within the Fallopian tube. As a result, it blocks the tube where the sperm and egg meet. Therefore, once Essure is embedded within the tube, the only way to remove it is by surgically removing the Fallopian tubes or the entire uterus (hysterectomy). The device needs to be removed intact so that fragmentation does not occur within the body. During its insertion, as the device is deployed from the uterine cavity into the Fallopian tube, a small portion of the device lies within the muscle of the uterus. Removing the Fallopian tube itself risks fragmenting the device. Hysterectomy is the safest and preferred surgical option, also recommended by the manufacturer.
Most hysterectomies can be safely performed through a minimally invasive laparoscopic route, with or without the robotic instruments. Laparoscopic or robotic hysterectomies are associated with less pain, bleeding, infection, formation of deep vein thrombosis and scar tissue formation compared to traditional open surgery. It also allows a quicker recovery. Hysterectomy is a major surgical procedure. There are potential risks of complications with any surgery. Hence, the pros and cons of having a hysterectomy for removal of Essure should be discussed with you before surgery.
Consulting with A Gynaecologist in Melbourne
If you are looking for an experienced gynaecologist in Melbourne to perform this procedure on you, or if you want to discuss whether you need to have your Essure contraceptive device removed, get in touch with our friendly team today.


